
Veterinary Review Initiative
This resource has been reviewed for accuracy and clarity by a qualified Doctor of Veterinary Medicine with farmed animal sanctuaryAn animal sanctuary that primarily cares for rescued animals that were farmed by humans. experience. The review process took place In February 2021.
Check out more information on our Veterinary Review Initiative here!
Check Out Our Basic Large BreedDomesticated animal breeds that have been selectively bred by humans to grow as large as possible, as quickly as possible, to the detriment of their health. Chicken Care Courses!
The following is an excerpt from Basic Large Breed Chicken Care Part 2, one of the free course offerings available at our Compassionate Care Classroom. We hope you will check out the course, but given how common mobility issues are in large breed chickens, we wanted to ensure this information is easily accessible to anyone looking for it by offering this stand-alone resource.
This information has been reviewed by a veterinarian as part of the development of the course.
Because of their large size and how quickly they grow, large breed chickens are very prone to arthritis and other mobility issues, even when their weight is appropriately managed. Obesity increases the likelihood that a large breed chicken will develop a mobility issue, can cause them to develop the condition earlier in life, and can exacerbate the issue, which is why managing their diet and their weight is so important.
Be sure to work with an experienced veterinarian if one of your chicken residents is showing signs of a mobility issue, which includes an uneven gaitA specific way of moving and the rhythmic patterns of hooves and legs. Gaits are natural (walking, trotting, galloping) or acquired meaning humans have had a hand in changing their gaits for "sport"., reluctance to bear weight, using their wings to help support them (which may cause damage to wing tips), or spending extended periods of time down (making them more prone to pressure sores). If individuals are very painful, they may also be seen open-mouth breathing (which can be a sign of being too hot or a sign of pain). While analgesics (pain medications) can help, it is very important to identify the cause of the mobility issue as well as manage any associated pain. In addition to performing a physical exam, your veterinarian may recommend imaging such as a radiograph or a CT scan to assess the cause of the mobility issue. Some of the more common causes of mobility issues in large breed chickens include:
Osteoarthritis (Degenerative Joint Disease)
Due to their large size, osteoarthritis tends to be a common issue in large breed chickens as they age, but individuals who are overweight could develop osteoarthritis at a younger age. Signs of osteoarthritis include abnormal gait, bearing weight unevenly when standing, lameness, and reduced activity. You may be able to hear or feel crepitus (grating or crunching) in the hock1: the tarsal joint or region in the hind limb of a digitigrade quadruped (such as the horse) corresponding to the human ankle but elevated and bending backward 2: a joint of a fowl's leg that corresponds to the hock of a quadruped (this can be more difficult to feel in the knee and hip). Chickens with osteoarthritis may spend more time lying down. Ensuring large breed chickens remain at a healthy weight can help prevent, or delay, osteoarthritis, but even chickens who are at a healthy weight could develop this condition. Treatment with analgesics and creating a living space that is easy for arthritic chickens to navigate can help keep residents comfortable.
Septic Arthritis (Infectious Arthritis)
Septic arthritis is inflammation of the joint(s) due to introduction of an infectious agent, which may result following septicemia or a localized infection of the joint. Large breed chickens appear to be more prone to septic arthritis than other chickens. In some cases, the joint may be red, swollen, hot, and possibly open and oozing. However, in other cases, there may not be obvious outward signs of infection, such as heat or significant swelling, and the chicken may look like they have a non-infectious mobility issue. Be sure to work closely with your veterinarian if a resident is showing signs of mobility issues and to discuss the possibility of septic arthritis. While your veterinarian may decide to tap the joint during their physical evaluation, this should not be attempted by anyone other than a veterinary professional- doing so could introduce bacteria into the joint and/or damage the internal structures of the joint, causing further issues. A veterinary diagnosis is imperative. Caregivers sometimes confuse clinical signs of gout with infection, and the two conditions require different treatments, so be sure to work closely with your veterinarian.
There are numerous pathogens that can cause septic arthritis, with Staphylococcus aureus being the most common. Other potential causes include Escherichia coli and Mycoplasma synoviae. Septic arthritis can be difficult to treat and typically requires prolonged systemic antibiotic treatment along with analgesics. Regional limb perfusion or the use of antibiotic-soaked gauze or impregnated beads may be recommended to deliver the antibiotics to the infected joint. Septic arthritis can cause permanent joint damage and predispose the individual to degenerative joint disease. Even following resolution of the infection, the individual may continue to have mobility issues and may require ongoing analgesics.
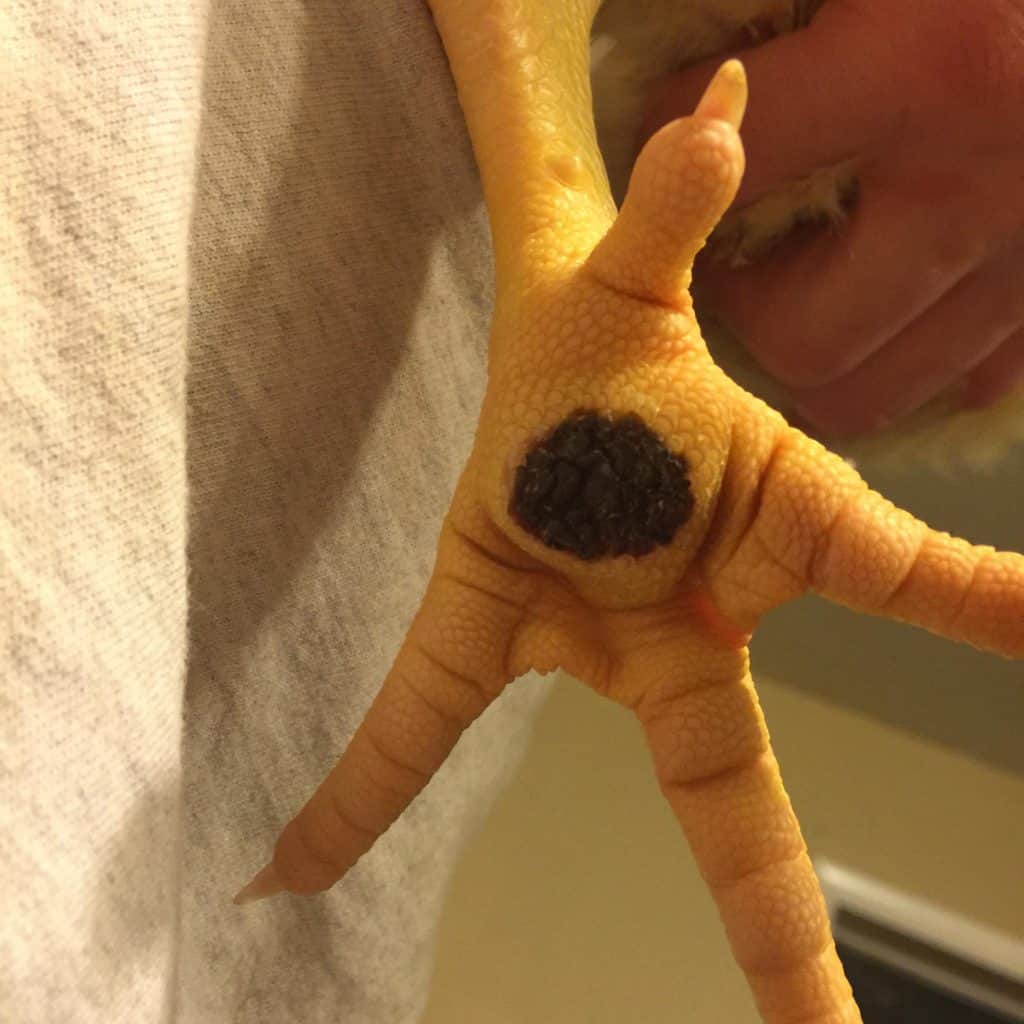
Bumblefoot (Pododermatitis, Foot Pad Dermatitis, Foot Pad Ulcers)
Bumblefoot can affect all breeds of chickens but is especially common in large breed individuals. Bumblefoot can be caused by many different factors including environmental conditions (such as poor sanitation or rough flooring or perching materials) or physical conditions (such as obesity or arthritis). Individuals who favor one foot over the other, due to pain or a mechanical leg issue, may develop bumblefoot on their “good” side. Because this foot has to bear more weight, the skin can become damaged over time. Without proper interventions, bumblefoot can progress from a minor issue to something far more severe.
Bumblefoot is typically categorized as mild, moderate, or severe, with severe cases involving infection in the bone (osteomyelitisan infectious usually painful inflammatory disease of bone often of bacterial origin that may result in the death of bone tissue.). The following 1-5 grading system gives a good overview of the progression of this disease and how it affects the overall prognosis, but be aware that your veterinarian may use a different grading system to evaluate and talk about bumblefoot.
Grade 1– At this stage, only the outer skin is affected. It may be very smooth (due to the loss of the small papilla normally present), and it may also be shiny and red, but there is no open wound or sign of infection. With proper interventions, prognosis at this stage is excellent.
Grade 2– At this stage, there is damage to the skin and there may be a scab, callous, or open wound, but the foot will not be obviously swollen. With proper interventions, prognosis at this stage is good.
Grade 3– At this stage, the disease process, and possibly infection, have progressed deeper into the tissues of the foot. The foot will be swollen and painful, and there may be discharge. Prognosis at this stage is good to guarded.
Grade 4– At this stage, the infection has progressed to involve deeper structures within the foot such as tendons and bone. Individuals with this stage of disease may develop tenosynovitis (inflammation of the tendon sheath), arthritis, and/ or osteomyelitis. Prognosis at this stage is guarded to poor.
Grade 5– At this stage, the condition is so severe that it results in debilitating deformity and loss of function. Prognosis at this stage is grave.
It is important to address bumblefoot early before it becomes actively infected and to prevent the introduction of bacteria by keeping the area clean and covered. Depending on the underlying cause, when caught early, foot wraps and changes to the environment may be enough to prevent progression if there is no infection. However, if the primary cause is osteoarthritis in the opposite limb, it can be very difficult to fully resolve bumblefoot and have the skin of the foot completely heal.
Be sure to work with a veterinarian if one of your residents has bumblefoot, especially if the affected foot is warmer than normal, painful, or swollen, or if it has discharge, an open wound, or a large scab. Your veterinarian can assess the foot to determine how severe the condition is (which may require x-rays), prescribe appropriate medications, and help create a treatment plan. Depending on the severity, treatment may include systemic antibiotics, analgesics, soaking the foot, various types of foot wraps, delivery of antibiotics directly to the affected area (for example, through the use of antibiotic-impregnated beads), and in some cases, surgical debridement (done by a licensed veterinarian with appropriate analgesics and anesthetics). Keep in mind that the individual’s good foot may be vulnerable to developing bumblefoot if they are especially painful and reluctant to bear weight on the affected foot. Be sure to keep a close eye on the other foot and protect it with a padded bandage as needed.
It is important to work with a veterinarian to determine which structures of the foot are affected, to establish an appropriate treatment plan, and if the treatment involves wound management or wrapping the foot, you must be shown how to do this properly. Left untreated, bumblefoot infections can have devastating consequences.
Other Mobility Issues
Just because one of your residents is limping, has an abnormality to their gait, or is spending more time lying down does not mean that they have one of the health challenges listed above. Chickens can develop mobility issues due to soft-tissue injury, neurological issues, or weakness from an underlying health issue. It is imperative you work with a veterinarian to determine the underlying cause and appropriate treatment plan.
Individuals with mobility issues may be at risk of developing pressure sores on their hocks and keel if they are spending prolonged periods of time down. Be sure to talk to your veterinarian about ways to protect against this, which may include environmental changes (such as additional bedding), padded bandages to offer additional protection, or the use of a device to support the individual while standing or walking (such as a sling or therapy chair).
To read more about Supportive Care For Non-Ambulatory Chickens, check out our resource here.
SOURCES:
Pododermatitis In Birds And Small Mammals | Schoemaker and Van Zeeland
Bumblefoot Surgery And Management | Great Western Exotic Vets
Backyard Poultry Medicine and Surgery: A Guide for Veterinary Practitioners (Non-Compassionate Source)
Noninfectious Skeletal Disorders in Poultry Broilers | Merck Veterinary Manual (Non-Compassionate Source)
Prevalence of Septic Arthritis Caused By Staphylococcus aureus In Poultry Birds At Tandojam, Pakistan | Journal Of Animal Health And Production (Non-Compassionate Source)
Mycoplasma Synoviae and other Associated Bacteria Causing Arthritis in Chicken | Tawfik, Khalil, Ellakany, Torky (Non-Compassionate Source)
Staphylococcosis in Poultry | Merck Veterinary Manual (Non-Compassionate Source)
A Multifaceted Approach to the Treatment of Bumblefoot in Raptors | J. David Remple (Non-Compassionate Source)






