
Veterinary Review Initiative
This resource has been reviewed for accuracy and clarity by a qualified Doctor of Veterinary Medicine as of January 2023.
Check out more information on our Veterinary Review Initiative here!
It’s an all too familiar situation that many new caregivers have experienced – you’re worried about one of your residents, so you have them evaluated by your veterinarian. After an exam and maybe some diagnostics, you’re sent on your way with medication in hand and a muddle of information in your head. Perhaps you’re not clear about your veterinarian’s diagnosis or if they even know for sure what is wrong yet. Maybe you’re unclear about what the medication you’re supposed to administer is actually for, and this can especially come into play if your veterinarian has prescribed more than one medication. To further complicate things, perhaps you’re also feeling unprepared to physically administer the medication if it’s something you haven’t been formally trained to do.
Between the worry and the waiting that sometimes accompany vet visits, not to mention the medical jargon, it’s easy to wind up feeling a bit unsure about the what, why, and how of a particular treatment. While we can’t help with the understandable worry you may feel about the individual in need of treatment, we can offer some tips to help ensure you leave vet appointments with the information you need to feel more confident when administering treatments to your residents.
It’s Not Just About Prescription Meds
While many medications require a veterinary prescription, some do not (as of this writing, there are even some commonly-used antibiotics that are available without a prescription, though this is in the process of changing). Just because you can head over to your local supply store or hit up an online supplier and get certain supplements or medications, this does not mean they should be used haphazardly. It’s still important to work with your veterinarian to ensure that 1) the treatment in question is appropriate given the circumstances and 2) that you are administering the treatment correctly. Using medications without veterinary advice could result in harmThe infliction of mental, emotional, and/or physical pain, suffering, or loss. Harm can occur intentionally or unintentionally and directly or indirectly. Someone can intentionally cause direct harm (e.g., punitively cutting a sheep's skin while shearing them) or unintentionally cause direct harm (e.g., your hand slips while shearing a sheep, causing an accidental wound on their skin). Likewise, someone can intentionally cause indirect harm (e.g., selling socks made from a sanctuary resident's wool and encouraging folks who purchase them to buy more products made from the wool of farmed sheep) or unintentionally cause indirect harm (e.g., selling socks made from a sanctuary resident's wool, which inadvertently perpetuates the idea that it is ok to commodify sheep for their wool). to your residents and, in the case of antimicrobials, can also lead to promoting antimicrobial resistance. We strongly recommend working closely with your veterinarian when making decisions regarding the administration of any supplement or medication.
Next, we’ll look at some of the important information you should gather next time your veterinarian makes treatment recommendations. While veterinarians may share some of this information without you having to ask, you may need to ask questions in order to leave with all the information you need.
What Is It?
Praziquantel, flunixin meglumine, tulathromycin, oxytetracycline… if these are not drugs you are familiar with, they may just look and sound like a jumble of letters. To further complicate things, much like how one might call a generic box of tissues “kleenex,” what your veterinarian says they are prescribing may not match with what’s written on the prescription or bottle of medication. Sometimes the brand name and drug name are close enough that you might figure out that they’re being used interchangeably (Metacam and meloxicam at least start and end with the same sounds), but other times it’s not so apparent (Banamine and flunixin meglumine, for example). Either way, it’s best not to make assumptions and to ask for clarification to ensure you’re going home with the correct medication and that you know what is what.
Knowing the name of the drug is just the beginning. It’s also helpful to understand what type of drug it is. While there are many types of drugs a veterinarian has at their disposal, the treatments that tend to come up most often usually fall into one of two categories: drugs that alleviate pain (analgesics) and drugs that treat or manage infection (antimicrobials and anthelmintics). Let’s look at both a bit more closely.
These Are Just Examples!
Below, we’ll talk about some different types of drugs and include examples of each. Please note that this is just to give you an idea of what drugs are included in each category. This is in no way meant to be treatment advice. Not all of the following drugs are appropriate in all species. Even if a particular drug can be used in a certain species, it may not be appropriate in certain situations or in certain individuals. Furthermore, the use of certain drugs may be limited or strictly curtailed by law. Always defer to your veterinarian regarding medication use.
Pain Medications
While certainly not the only type of medication used to alleviate pain in farmed animal sanctuaryAn animal sanctuary that primarily cares for rescued animals that were farmed by humans. residents, non-steroidal anti-inflammatory drugs, often referred to as NSAIDs, are most commonly used. Examples of NSAIDs include carprofen (sometimes referred to by the brand name “Rimadyl” or “Novox”), meloxicam (“Metacam”), flunixin meglumine (“Banamine”), and phenylbutazone (“Bute”). As mentioned above, not all of these drugs are appropriate to use in all species. NSAID treatments should never be combined with other NSAIDs or steroids (such as dexamethasone), and in some individuals, NSAID use may be contraindicated (not advised). Depending on the situation, your veterinarian may do blood testing prior to prescribing an NSAID, and/or they may recommend blood testing later on to check for adverse effects. In some cases, your veterinarian may prescribe a controlled opioid (for example, tramadol) or a drug for nerve pain (such as gabapentin) either in place of or in addition to an NSAID.
Your Vet Needs Info From You, Too!
While the focus of this resource is on the information you need from your veterinarian when tasked with administering treatment to one of your residents, there is a lot of important information your vet needs from you as well. Oftentimes, they will ask for this info or, if they are your primary vet, they may have some of this information in their records from previous visits. Of particular note, it’s important that your veterinarian is made aware of any current or recent treatments the individual has received; any allergies or adverse reactions they’ve had to medication in the past; and their general health history, including any chronic conditions they have.
Antimicrobials And Anthelmintics
Like humans, farmed animalA species or specific breed of animal that is raised by humans for the use of their bodies or what comes from their bodies. sanctuary residents can develop infections caused by different types of organisms, such as microorganisms (bacteria, viruses, fungi, and protozoa) or helminths (parasitic worms). Drugs used to kill or slow the growth of these organisms can be categorized by the type of organism(s) they work against and include:
- Antibiotics – Used for bacterial infections (examples include amoxicillin, doxycycline, and tulathromycin)
- Antifungals – Used for fungal infections (examples include nystatin, itraconazole, and fluconazole)
- Antiprotozoals – Used for protozoal infections (for example, amprolium)
- Anthelmintics (dewormers) – Used to treat parasitic worm infections (examples include fenbendazole, ivermectin, and levamisole)
Though sanctuary residents can certainly develop viral infections, antiviral use is not as common in veterinary medicine and, in some cases, is strictly prohibited. This is due, in part, to the concern that antiviral use in non-human animals, and particularly in species the FDA labels as “food animals,” contributes to the development of antiviral resistance in viruses that affect humans.
Drug Resistance
While you should be sure to follow your veterinarian’s instructions for all medications, regardless of their type, it’s important to stress that improper use of antimicrobials and anthelmintics can contribute to issues of drug resistance, which is a concern globally. While this issue is not unique to antibiotics, antibiotic-resistant bacteria are a serious concern that could put both humans and non-humans at risk. Be sure to follow your veterinarian’s instructions regarding dosing and duration of antimicrobials and anthelmintics. It is important to finish the entire treatment course, even if the symptoms have resolved, and it is important to make sure you do not skip any doses unless so instructed by your veterinarian. If you are coming toward the end of the prescribed treatment, and the individual’s symptoms have not resolved, check in with your veterinarian before you discontinue the treatment. They may recommend continuing the treatment a bit longer.
Why Do They Need It?
In addition to knowing what the drug is, you also want to know why they need it. While this may seem obvious, it’s not always as straightforward as you may assume. While you may be prescribed a medication to treat the primary issue (ex. an antibiotic to treat a bacterial infection), medications may also be prescribed for a variety of other reasons, such as managing specific symptoms (ex. prescribing a medication to stimulate appetite); treating or preventing secondary issues (ex. using antibiotics to treat a secondary bacterial infection even though the primary issue is viral); or to prevent or manage side effects caused by another medication (ex. prescribing a gastroprotectant along with a medication that has the potential to cause ulcers).
If your resident has been diagnosed with (or is suspected of having) more than one condition that requires treatment, it’s also helpful to understand which treatments are for which condition. While you may wonder why any of this matters, knowing this information can help you in terms of deciding what and when information needs to be communicated to your veterinarian (which may come into play when trying to figure out refills) and can also be useful in terms of record keeping.
How Is It Administered?
Proper administration of medications is of the utmost importance. Before leaving the vet appointment, be sure you fully understand how to administer any treatments that have been prescribed. Improper administration can result in various issues depending on the treatment and administration route. To ensure you are prepared to administer the treatment at home, we recommend asking your veterinarian to explain, then demonstrate, and then watch you while you replicate what they have shown you. This will give them the opportunity to provide feedback and will give you the opportunity to ask for clarity if needed.
Teaching drug administration is beyond the scope of this resource, but we do want to highlight some of the more common routes of administration you may come across. These include oral, topical, or injectable forms.
- Oral – Treatments that are administered orally (by mouth, sometimes abbreviated as “PO”) can come in different forms, such as tablets, capsules, liquid suspensions, pastes, or powders.
- Topical – Topical treatments are administered to the skin or mucous membranes. Topical treatments can come in many different forms, such as dusting powders, ointments, or gels that are applied to the skin or solutions such as eye or ear drops. Some topical treatments provide localized treatment, while others are absorbed and have a broader effect.
- Injectable – While there are additional types of injections, in terms of treatments you’ll be asked to administer at home, you’ll most often come across treatments that are administered subcutaneously (under the skin, abbreviations include SC, SQ, sub-Q, and subcut) or intramuscularly (into the muscle, abbreviation IM). In some cases, particularly if an individual has had a catheter put in, you may be asked to administer medication intravenously (into the vein, abbreviation IV).
Additional Caution When Administering Injectable Treatments
While proper administration is important for any medication, if you are instructed to administer an injectable medication, it is imperative you learn how to do so safely. Improper administration could have grave results.
If you have concerns about the feasibility of a particular administration route or are worried about the potential stress it may cause the individual in question, be sure to ask if there are other options. Sometimes there simply aren’t, but you might just find that there are other options to consider. For example, if your veterinarian prescribes an injectable medication for one of your pig residents and you have concerns both about your ability to administer this and also the pain and stress an injection will cause, you can ask if there is an oral alternative. To offer another example, because of the risk of aspiration with oral liquid suspensions, if one of your turkeyUnless explicitly mentioned, we are referring to domesticated turkey breeds, not wild turkeys, who may have unique needs not covered by this resource. residents is prescribed a large volume of an oral liquid medication, you can ask if there is an appropriate treatment that comes in a tablet or capsule.
Unfortunately, sometimes there’s not an appropriate substitution, in which case you must work with your veterinarian to make sure you are comfortable administering the prescribed treatment. You can also consider ways to make the treatment less stressful and add a positive element to it (such as a tasty treat following administration).
Whatever The Administration Route, Be Sure You Have The Necessary Supplies
Before going on your way, make sure you have any supplies that are needed for administration of the medication. For example, some oral medications may need to be administered with a special tool(s). Depending on the tool needed, this may be something your veterinarian provides or something you need to pick up at your local pharmacy or farm supply store. You may also be prescribed a medication that needs to be reconstituted or diluted, in which case you must make sure you have the supplies necessary to do this. Injectable medications require specific tools, described below.
Supplies For Injections
Injectable treatments typically require a needle and syringe, but may also require additional supplies depending on the treatment and the species of the individual. In some cases, particularly if only a few small doses are necessary, your veterinarian may draw up these doses for you, providing the appropriate amount of medication in appropriately-sized syringes attached to appropriately-sized needles. Other times, you’ll be provided with a vial of medication and the necessary needles and syringes. If you have a stash of unused needles and syringes from previous treatments, make sure you understand how these are sized before making the assumption that you do not need the needles or syringes your veterinarian provides.
Needles come in different lengths and gauges (size of the needle opening). The appropriate size will depend on a variety of factors, including the species and size of the individual, the viscosity of the medication, and the administration route. For example, using a needle that is too long for an intramuscular injection in a chicken resident could result in the medication being injected into the body cavity rather than into the muscle. Needle gauge refers to the size of the needle opening. As the gauge increases, the size decreases (i.e. a 25-gauge needle is smaller than an 18-gauge needle). Generally, it’s best to use the smallest gauge possible, though what this equates to will vary by species and will also depend on the thickness of the drug. Very thick drugs may require a bigger opening (lower gauge) than what you would typically use in a particular species. Your veterinarian can advise you regarding the most appropriate needle size for each situation. If you plan to use your own supplies for injections, be sure to ask for more information regarding the needle length and gauge your veterinarian recommends so you can ensure you have what you need.
Syringes also come in different sizes based on the amount of liquid they can hold. It’s often easiest to use a smaller, rather than a larger syringe. For example, when administering a small amount of medication, maneuvering a 1cc or 3cc syringe will be easier than if you are using a 20cc or 60cc syringe. It is important you understand how much you’re drawing up in the syringe, as misreading or misunderstanding the syringe amount can result in harm to your residents. Accurate measurement will be easier if you use the smallest syringe possible. That being said, it’s best not to push a syringe to its limit, if possible. The plunger of a full syringe can easily be knocked out, spilling the syringe’s contents, or it can be inadvertently depressed, resulting in some of the medication being expelled before administration. In the case of larger syringes, it can also be difficult to maneuver a full syringe and put enough pressure on the plunger while keeping the needle in a steady position.
In addition to different sizes, syringes for injections come in Luer lock and Luer slip types. Luer lock syringes are designed so that the needle twists and locks onto the end of the syringe, whereas a Luer slip syringe does not lock onto the needle. Medical professionals prefer one over the other depending on the task at hand, but for subcutaneous and intramuscular injections, you may find that the Luer lock syringe is your best bet. When using a Luer slip to administer medication, it is easy to create so much pressure that the needle detaches from the syringe, spraying medication all over the place. There are also other types of syringes that are not intended for injections and do not have appropriately sized tips to attach to a needle.
How Much Do They Need?
In addition to understanding how to administer the medication, make sure you understand how much to give them at a time. Over- and under-dosing can both cause issues, with severity depending on the medication and the amount given. If your veterinarian gives you dosing instructions that require you to calculate the exact dose, this must be done very carefully. You can read more about how to do this here.
Whether the dose is relayed to you verbally or in writing, it can be helpful to repeat this information back to your veterinarian to ensure you have the proper dose. Errors can occur for all sorts of reasons, including mishearing or misreading the information or can be the result of a communication issue between the prescribing veterinarian and the person filling the prescription. According to the FDA, one common cause of medication errors is the misinterpretation of abbreviations. For example, misreading “mcg” or “µg” (microgram) as “mg” (milligram) will result in a dose that is 1000 times higher than intended. Another common dosing error results from the omission of leading zero or the addition of trailing zeros, causing people to miss the decimal point. For example, if a dose of 0.1 is written as .1, it may be misread as 1. Similarly, if a dose of 1 is written as 1.0, it may be misread as 10.
Repeating the dosing info back to your veterinarian helps ensure you know the proper dose and can help avoid issues with misinterpretation (especially if the dosing information is handwritten). It can also help you catch an issue that has nothing to do with you (for example, you may notice that the information provided by the pharmacy does not match what your veterinarian told you). Any time you are unsure about how much medication to give, contact your veterinarian for clarification.
Write It Down
In addition to repeating information back to ensure you have the right information, we recommend taking notes to ensure you remember this information. Animal caregivers tend to have a lot they need to keep track of, and, unfortunately, our memory isn’t infallible.
In some cases, you may need additional supplies in order to accurately measure each dose. This may include a sharp knife or pill cutter to divide tablets if you are to administer only a portion at a time, or you may need instruments such as measuring spoons, syringes, or even a small scale. Make sure you have the supplies necessary to accurately measure the medication.
Measuring Liquid Medications
If you need to measure out a liquid medication using a syringe, make sure you know how to do so properly. Be sure to use the top of the plunger stopper (the end that is closest to the syringe tip) to measure how much you are drawing into the syringe. Using the other end of the stopper (the part that attaches to the plunger) to measure will cause you to draw up an inaccurate amount.
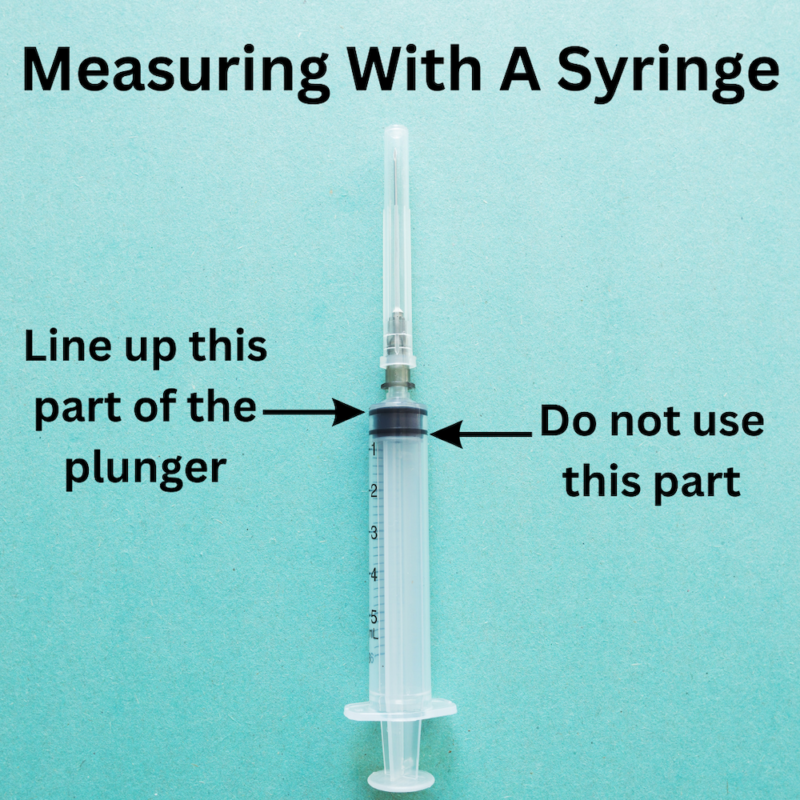
If the medication is clear, it can be difficult to tell if you are drawing air or medication into the syringe, particularly if you are only drawing up a small amount. Pay close attention to ensure that you have drawn up the correct amount of medication, and watch for air bubbles, as they will cause you to administer less medication than intended.
If your veterinarian prescribed dosing instructions in milliliters (ml), but the dosing syringe measures in cubic centimeters (cc) or vice versa, have no fear! Milliliters and cubic centimeters are equivalents when it comes to measuring volume.
How Often Do They Need It?
In addition to knowing how much of the medication should be administered at any one time, you also need to know how often it should be administered. For example, do they need the medication once, twice, or three times per day? Or perhaps it is only administered once every X number of days. Some treatments may require that you administer the treatment for a certain number of consecutive days followed by a certain number of days when the medication is not given (for example, a medication may be prescribed for three consecutive days each week, resulting in the treatment being due every Monday, Tuesday, and Wednesday, with no treatment administered between Wednesday’s dose and the following Monday’s dose).
Understanding how often the medication should be administered goes beyond just knowing how many times per day or week to administer the medication. Make sure you also understand when treatments should be administered. Often this will be based on the time between doses (so, for medications that are to be administered twice daily, this typically means spacing doses out to be approximately 12 hours apart). Your veterinarian may also recommend a specific time of day the medication should be administered (such as first thing in the morning, with their breakfast, or just before bedtime, for example). Other times, administration may depend on other activities or treatments. For example, you may be instructed to administer a medication X minutes before the individual eats. Or, in the case of multiple medications being administered, you may be instructed to space out certain treatments following a very specific schedule (i.e. after administering drug A, wait at least 2 hours before administering drug B).
Depending on the treatment and situation, you may be instructed to give the medication “as needed” with stipulations about the maximum frequency and dose that can be used. So, perhaps the treatment can be administered once per day at most, but you are instructed to give it only when you observe certain signs or behaviors (ex., you only give the medication if they are not eating well, but can give it no more than every 24 hours). Do not follow the “as needed” plan unless your veterinarian has instructed you to do so, as this is not appropriate for many treatments.
As with understanding how much they need, when it comes to how often they need the treatment, we recommend repeating the instructions back to your veterinarian to ensure you understand. In addition to the communication issues mentioned above regarding dosage amounts, misreading or misinterpreting abbreviations pertaining to frequency has also occurred. For example, SID (intended as “once per day”) has been misinterpreted as BID (twice per day) and QID (four times per day), and the abbreviation TIW (three times per week) has been misread as TID (three times per day). These misinterpretations can have serious consequences depending on the medication being administered. Repeating your veterinarian’s instructions back to them can help avoid these issues.
To avoid misinterpretation of abbreviations at your sanctuary, you may want to write out all instructions in full rather than using abbreviations. If you do choose to use abbreviations, we recommend ensuring everyone preparing and/or administering treatments is properly trained in how to read abbreviations. It can also be helpful to have a list of abbreviations and their meanings posted for reference.
Contact Your Veterinarian Immediately In The Case Of Overdose
If one of your residents is given too much medication, be sure to contact your veterinarian immediately. They can instruct you on any immediate steps to take, and if the individual is to be observed for adverse effects, your veterinarian can tell you what signs to watch for and what to do if they are observed.
For How Long Should You Administer It?
In addition to dosing frequency, you also need to know how long to administer the treatment. Some treatments may be prescribed until a follow-up appointment or recheck diagnostics. Others may have a set number of doses or days they are to be administered, or you may be offered a range with instructions to administer treatment at least X days, but not more than Y days (i.e. if the treatment is to last 7-10 days, you would not stop administering the treatment before the 7th day or go beyond the 10th day without instruction from your veterinarian). Some medications should not be stopped abruptly and instead require gradually decreasing the daily dose following your veterinarian’s instructions.
Having a clear understanding of how long to administer the medication (and also understanding the type of medication and its purpose) is not only important in terms of making sure you are properly following your veterinarian’s instructions, it also helps when figuring out if you need to request a refill.
Requesting Refills
Make sure you know how to go about requesting a refill. In some cases, your veterinarian may have prescribed a certain number of refills, in which case, requesting a refill may simply mean calling your vet clinic and talking to a receptionist or calling the pharmacy, depending on where the prescription was filled. Even though you can request these refills without having a conversation with your veterinarian, there may be some lag time between your request and the medication being ready to pick up or ship. Make sure you have these details in advance so you can avoid running out of medication before you receive the refill. In other cases, the prescription may not have any refills, in which case you will need to talk with your veterinarian to see if it is appropriate for the individual to continue the treatment. Depending on the circumstances, your veterinarian may want to recheck the individual before making further recommendations. In either case, it’s wise to plan ahead as much as possible.
Are There Potential Side Effects You Should Watch For?
Almost all medications carry some risk of side effects, but some carry more risk than others, and some carry more severe potential side effects than others. It’s a good idea to ask if there are certain side effects you should be on the lookout for and what (if anything) you should do in response if these side effects develop. For example, your resident may be prescribed medication that can make them sleepy or less active than usual. While this reaction may not be so severe that further steps are needed, it’s helpful to know this is a possibility so that you are able to recognize this change in behavior as likely related to their medication. Other times, more severe side effects may be possible and warrant action on your part. For example, if one of your residents is on medication that has the potential to cause a gastric ulcer, you may be instructed to discontinue treatment and contact your veterinarian immediately if they show signs of an ulcer.
If you are ever unsure if what you are seeing in a resident can be attributed to a medication they are on, we recommend getting in touch with your veterinarian. Similarly, if you feel you are seeing a more severe manifestation of an expected side effect and have concerns, contact your veterinarian for guidance.
Are There Any Special Instructions?
In addition to the above, make sure you are aware of any special instructions associated with the storage, preparation, administration, or disposal of the medication. For example, while most medication should be stored in a cool, dry place and secured so that residents/companion animals and children cannot access them, some medications require more specific storage, such as refrigeration or protection from sunlight. It’s also important to understand how long the medication lasts. Medications that require reconstitution typically have a specific (and often relatively short) shelf life following reconstitution, so it’s important to keep track of when the medication was reconstituted and when it needs to be discarded. Speaking of discarding medication, be sure to discard medications in the correct way, which will depend on the medication. Your local pharmacy might take back medications or be able to point you in the direction of drug take back programs in your area. In the case of controlled substances, your veterinarian may provide more specific instructions for disposal.
It’s also important to be aware of and follow any special instructions related to the administration of medications. Some of this was already discussed above, such as understanding if the medication needs to be administered with food or timed with other treatments. In addition to these considerations, you also want to be aware of and understand special instructions related to human safety. For example, should humans handling the medication wear gloves or other protective gear? Also, keep in mind that some medications may not be safe for certain folks to come into contact with. For example, folks with certain allergies or other medical conditions or who are pregnant or breastfeeding may need to take extra precautions when handling certain medications or may need to avoid handling certain substances entirely. This is important information to have and to share with anyone who may come into contact with the medication.
Keeping Track Of It All
Once you have all the information you need, make sure to put it in writing and clearly communicate it to everyone who needs it. Even if you are the sole person in charge of administering the treatment, it’s still important to get the important information in writing rather than relying on memory alone. We recommend using our Ongoing Treatment And Observation Record or a similar system to keep track of pertinent information.
SOURCES:
Your Pet’s Medications | American Veterinary Medical Association
Routes Of Administration And Dosage Forms | Merck Veterinary Manual
Antimicrobial Resistance | World Health Organization
A Microgram Of Prevention Is Worth A Milligram Of Cure: Preventing Medication Errors In Animals
Overview Of Antifungal Agents For Use In Animals | Merck Veterinary Manual
Using Medication: Topical Medications
Measuring Liquid Medications | Compounding Solutions
Medically Important Antibiotics To Move From OTC To Rx | American Veterinary Medical Association (Non-Compassionate Source)
Overview Of Antiviral Agents Used In Animals | Merck Veterinary Manual (Non-Compassionate Source)
Non-Compassionate Source?
If a source includes the (Non-Compassionate Source) tag, it means that we do not endorse that particular source’s views about animals, even if some of their insights are valuable from a care perspective. See a more detailed explanation here.








